Claim denials, administrative overload, and rising operational costs continue to challenge healthcare providers, making efficient eligibility checks more important than ever. Manual verification methods—such as repeated calls to payers, navigating multiple portals, and re-entering patient data—slow down workflows and often introduce costly errors. These inefficiencies directly impact revenue cycles and create delays in patient care.
A large share of denials originates from incorrect or incomplete insurance details captured at the time of registration. As payer rules become more complex, maintaining accuracy without automation becomes increasingly difficult for healthcare teams.
Modern insurance verification software addresses these challenges by automating eligibility checks, validating coverage in real time, and integrating seamlessly with existing healthcare systems. This reduces manual effort, improves data accuracy, and ensures faster claim processing.
In this guide, we’ll explore the top tools available, their key features, and how they can help healthcare organizations improve efficiency, reduce denials, and strengthen revenue cycle performance.
What is Insurance Verification Software?
Insurance verification software is a computer-based program that is mostly employed in the healthcare industry to automate the process of ensuring that a patient has insurance, meets the eligibility requirements, benefits, deductibles, co-pays, and prior authorization in real time. It offers the opportunity to combine with electronic health records (EHRs), practice management systems (PMS), and payer databases of hundreds of insurers, including Medicare, Medicaid, and commercial providers, to eradicate manual calls and paperwork and retrieve the correct information, including out-of-pocket costs, excluded plans, and claim statuses, in seconds. This lowers the number of errors, denial of claims, administrative costs, and risk of fraud and accelerates the process of managing revenue cycles, booking appointments, and billing providers.
The Problem With Traditional Insurance Verification
Conventional verification of insurance is done manually, thus posing inefficiencies and risks in a healthcare environment. Such techniques tend to result in time wastage, mistakes, and losses to the providers.
Key Problems:
- Time-intensive activities: There is a 10-15-minute per-patient call, fax, or portal log-in time that creates bottlenecks in high-volume practices.
- High error rates: Manual entry results in 18-27% errors, such as transposed policy numbers, incorrect deductibles, or omission of coverage limits, which causes the denial of claims.
- Lack of consistency in standards: Checking of verification is not always carried out by the same staff, as some may not be able to check their benefits or network status due to time constraints.
- Stale information: 38% of denials and loss of revenue are due to outdated information coverage (e.g., Medicare shift mid-month).
- Lack of complete data: The absence of patient information or dissonance in policies leads to the duplication of work and billing errors.
- Burnout among staff: Monotonous work wears down the staff, and turnover rises, and the focus on patients is lost.
- Sluggish reimbursements: Understandings and ambiguity on exclusions result in denied claims, rework, and payment problems.
Why Modern Practices Are Switching to Automated Insurance Verification Software?
Automated verification software is becoming popular in modern healthcare and insurance practice as it allows streamlining operations and reducing costs.
Key Reasons for the Switch
- Cuts claim rejection rates and errors by 99.5% over 80-85% with manual procedures.
- Reduces time spent on cuts by 4-6 minutes per patient, increasing employee productivity on higher value work.
- Allows real-time eligibility verification, including immediate coverage information, copayments, and deductibles.
- Avoids the rejection of claims by 20-30% at a saving of 25-50 per claim and enhancing cash flow.
- Cuts down administrative expenses by 40-60% using less manual effort and follow-ups.
- Increases patient satisfaction through prompt check-in and billing, and reduces surprises.
- Gives active notifications regarding the change of the policy and expiry to avoid leakage of revenues.
- Make HIPAA compliant and liberate personnel to attend to patients.
List of Top 12 Insurance Verification Software
1. Experian Health
Experian Health Insurance Verification tool is a web-based medical software that automatically verifies real-time insurance-eligibility and benefits data on the providers to minimize claims rejection and expedite payment via access to a huge network of payers. It is compatible with EHRs and practice-management systems, and gives real-time coverage status, copays, and deductibles to staff when they are at the point of service, as well as coinsurance and pre-authorization requirements. It also helps in searching Medicare MBI and bad-plan-code identification and standardized eligibility results via the site, which means that the billing departments can find out the issues early and improve the accuracy of the revenue cycle.
Key features:
- Live insurance eligibility and benefits checks on thousands of payers.
- Back-up payer connectivity eligibility clearinghouse to decrease service outages.
- Validation and lookup of Medicare Beneficiary Identifier (MBI).
- BadPlanCode (BPC) identification to indicate bad or mismatched plan codes and reduce denials.
- Integration with EHRs, practice-management, and EDI/API-based billing systems.
- Prior-authorization and claims status in the same workflow.
- Denial trend and revenue-cycle performance reporting and analytics.
Pros:
- Eliminates manual verifications and front desk mistakes drastically.
- Reduces claim denials and enhances the predictability of cash flow.
- Wide payer network and close to real-time response rate.
- Powerful interoperability with other existing health-IT systems.
Cons:
- Smaller practices can be priced in the high range (they are often estimated at hundreds of dollars per provider per month).
- Initial configuration and integration can be extremely implementation-intensive and costly in terms of consulting.
- Mostly oriented to U.S. revenue-cycle processes, and therefore not very useful to the non-U.S. providers.
Price:
Usually, pricing is by request
Website:https://www.experian.com/healthcare/
2. Spry Insurance Verification Software
Spry Insurance Verification Software is a real-time software, which is an artificial intelligence (AI) based eligibility-checking software that is integrated with the SPRY EMR/EHR software that is mostly found in physical therapy and allied-health clinics. It automates intake insurance verifications, and retrieves detailed benefit information (deductibles, copays, prior-auths required, and limits on the number of visits), and it cross-relates directly with the scheduling and billing process, such that the eligibility, authorization, and claims scrubbing are collaborating, at least within the same workflow, without the need to perform manual work and claim rejection.
Key features:
- Instantaneous eligibility checks on insurance with a real-time payer-portal.
- There is more accuracy and reduced errors in automation and claim scrubbing by AI.
- Unlimited tests (no-per check fee) on subscription.
- Detailed information on specific benefits of PT: deductibles, copays, prior-auth requirement, and visit restrictions.
- Automatic compliance (e.g., KX modifier to Part-B Medicare) to reduce rejections.
- End-to-end revenue cycle integration. Smooth integration with SPRY EMR, scheduling, and billing.
Pros :
- On-the-spot checks of eligibility conserve time at the front desk.
- Measurement (Greater than 95%+) lowers claim rework and denials.
- No per-check charges to decrease the cost of the long-term verification.
- In conjunction with the EMR, billing, and scheduling; less data entry.
- Detailed benefit description improves patient financial-responsibility conversations.
Cons:
- Other users have also complained of the occasional glitches in their billing or claim-processing.
- Some parts of the system might be slow when dealing with the interface or require pages to refresh.
- Therapy/ambulatory-care primarily maximized; not necessarily applicable to all kinds of specialty out-of-the-box.
- Lack of transparency of accurate prices; it is usually given on a case-by-case basis.
Price:
Quote-based
Website: https://www.sprypt.com
3. Waystar
The Waystar Insurance Verification tool is a revenue-cycle/ eligibility-verify software running in cloud computing, which is applied in healthcare organizations to automate insurance eligibility, identify concealed/secondary coverage, and minimize claim denials before the service delivery. It is related to practice-management and EHRs to retrieve patient-data, make real-time or batch eligibility requests to thousands of payers (Medicare and most commercial plans), and offer coverage data, benefit limits, and risk notification during registration or in pre-admission, so that employees can rectify errors and gather patient responsibility at admission.
Key features:
- Live and large-scale insurance eligibility of individual patients or huge groups.
- Coverage Detection This detects automatic coverage of hidden or unknown insurance (including second plans and coordination-of-benefits situations).
- Smart notifications on inactive policies, coverage holes, plan exceptions, and other payer-risk indicators to avoid denials.
- MBI look-up and plan-code matching to minimize medication errors and bad-debit write-offs.
- Ability to create customizable dashboards and reports to monitor performance or verify verifications, denials, and coverage captures.
- Cloud-based clearinghouse/RCM software that facilitates claim scrubbing and rejection management, and resubmission processes.
- Connection to large EHRs and practice-management systems and AI-based data normalization to facilitate workflow.
Pros:
- Eligibility and coverage checks are fast, partially automated, so that less time is spent on manual work and staff.
- Identifies and corrects coordination-of-benefits problems, enhancing reimbursement, and catches hidden or secondary insurance.
- MBI-lookup and proactive alerts prevent denials and minimize write-offs related to Medicare.
- High-quality payer connectivity and effective integration with numerous EHR and practice-management systems.
- Revenue-cycle analytics dashboards and reporting.
Cons:
- Not every plan or niche is supported; there are still some that need to be verified manually.
- In some cases, glitches or downtimes might disrupt the eligibility processes.
- Pricing and feature levels may be complicated, and sophisticated features (e.g., sophisticated RCM tools) increase the price.
- IT and workflow installation and training of the staff are necessary to get the full benefit.
Price :
Based on a customized contract
Website:https://www.waystar.com
4. Verify Treatment
VerifyTreatment To VerifyTreatment is a health insurance verification site with providers of behavioral health, addiction treatment facilities, mental health facilities, and skilled nursing operations as its main target audience. It eases the insurance eligibility background by incorporating real-time checks on more than 1,700 payers, enabling admissions staff to swiftly evaluate coverage facts such as deductibles, co-pays, and benefit constraints and authorization requirements to avoid insurance claim denials and loss of revenue. The software enables mass authentication of full patient censuses, mobile operations to build an on-the-job workflow, HIPAA-compliant tools to collaborate, and connections, such as Salesforce, to achieve the integrity of data in CRM systems.
Key Features:
- Eligibility values that are verified in real time on 1,700+ payers with full benefits information.
- Mass verification and automatic re-checking with policy lapse notifications that can be customized.
- Web access, mobile app (iOS/Android), and 24/7 access to remote teams.
- Payer risk flagging, status/ERA tracking, claim, and compute co-pay/deductible.
- HIPAA Compliance, customizable dashboards, reports, and self-service checks on the coverage of the patients.
- CRM integration and Salesforce compliance logging on Joint Commission standards.
Pros:
- Denies through proactive warnings.
- Quick and precise in the event of behavioral health.
- Multi- and mobile-support.
Cons:
- There are a few user reviews/ratings.
- The emphasis on behavioral health can restrict the general use of medicine.
Pricing:
Pricing is non-public, and it has to be contacted and asked to be quoted individually.
website: https://www.verifytx.com.
5. Optum Coverage Insight
Optum Coverage Insight is a software program that can be used to discover and verify the insurance of patients who were either listed as self-pay or underinsured to aid in minimizing bad-debt losses and enhance revenue-cycle performance. It applies data mining, machine learning, and predictive analytics to cross patient demographics and histories with the payer networks, and indicates possible additional coverage (commercial, government, and exchange plans) prior to or following service.
Key Features:
- Determines the existence of undisclosed/unclaimed insurance cover of self-pay or underinsured.
- Connects with payer networks to authenticate insurance and demographic data on a real-time basis.
- Facilitates pre-service and post-service coverage analysis to minimize the number of denials and enhance collections.
- Dstreams predictive analytics and machine learning to rank and rank potential coverage matches.
- Has suppression characteristics to curb identity-fraud risk in the coverage discovery.
- Integrates with the current registration and revenue-cycle processes (EHR/RCM systems) through batch or API-style integration.
Pros:
- Gather more revenue by locating other coverage that self-pay patients have missed.
- Write off and bad debt through validation of the status of true uninsured.
- Does not disrupt workflow as it integrates with current payer networks and EHR/RCM systems with minimal workflow.
Cons:
- Budgeting may be opaque because pricing is usually tailored and is not publicly listed.
- It is effective based on the quality of data and payer-network coverage, and, therefore, outcomes can be different across regions and specialties.
- It may need IT and revenue-cycle support to implement and integrate with legacy systems.
Price:
There is no fixed price per-user or per-transaction
Website:https://marketplace.optum.com
6. CERTIFY Health
CERTIFY Health Insurance Verification Software is a cloud-based solution designed specifically for healthcare providers such as hospitals, clinics, and practices to automate and streamline real-time patient insurance eligibility checks, eliminating claim denials and quickening the revenue cycle through manual processes that had previously been automated. It is integrated with electronic health records (EHR), practice management systems (PMS), and electronic remittance advice (ERA) solutions of the leading vendors, including EPIC, Cerner, and Athenahealth, and retrieves information on the coverage, co-pays, deductibles, and out-of-pocket estimates in real-time and puts them at the point of patient intake or scheduling.
Key Features
- Benefit, coverage, and authorizations. Payers using a one-click verification query are instantly charged through payer portals, whether at check-in or on-scheduling.
- Calculates the patient responsibility (deductibles, co-insurance, co-pays) and creates valid estimates to facilitate initial collections.
- Integrates with EHR/PMS/EMR systems, APIs, and HL7 protocols, with bidirectional data flow without impacting work processes.
- Processes and verifies high-volume surgeries or big practices, including denial prediction, scrubbing, and proactive alerts.
- Self-service Provision: Patients have the option to check their own coverage through secure links, eliminating the need to call the front desk.
- Monitors verification rates, denial rates, and ROI rates to manage the revenue cycle most effectively.
Pros:
- Eliminates denials and decreases verification time (from hours to 2 minutes).
- Improves cash flow, reduces work load in staff, and reduces burnout.
- Growing from small to large hospitals.
Cons:
- Custom pricing involves sales quotes; no open, transparent levels.
- The initial setup and integrations could require IT support (1-4 weeks).
- It may have sporadic API downtimes, depending on the accuracy of payer data.
Pricing:
Quote-based
Website:https://www.certifyhealth.com
7. Inovalon Insurance Discovery
Inovalon Insurance Discovery is a SaaS insurance-coverage discovery and eligibility-verification cloud-based application that assists healthcare providers in determining active, billable insurance of patients who seem uninsured or underinsured. It will minimize uncompensated care, decrease claim denials, decrease days in accounts receivable, and recover unbilled revenue through running real-time and high-volume batch searches in national payer databases and by using algorithms and EDI-style eligibility checks. The tool can be combined with the EHRs and the overall data ecosystem of Inovalon, which makes it applicable to large hospitals, health systems, and provider networks requiring scalable insurance-discovery workflows that are compliance-oriented.
Key features
- Recognizes active primary, secondary, and tertiary insurance by managed care, Medicare Advantage, and commercial plans.
- Conducts real-time and high-volume batch automatic study of patient files.
- Calculates national payer information and proprietary algorithms used to identify coverage and conduct eligibility checks.
- EHR-integrates (e.g., Epic, Cerner, Meditech) with the Inovalon ONE platform/data lake.
- Tracks Medicare MBI and other payer identifiers, as well as aids in ongoing reassessment of the coverage status.
- Helps will decrease the days in A/R, denials, and self-pay balances and enhance patient financial transparency.
Pros:
- Expands the number of hits of previously uninsured or underinsured accounts.
- Minimizes uncompensated care and collects delayed revenue before deadlines of timely-filing.
- Automate works throughout the revenue cycle (pre-, point-, and post-service) with little manual work.
- Scalable to small or large health systems and multi-facility systems.
Cons:
- May be hit-and-miss to selected payers or coverage types based on the quality of the data feed.
- Mainly focused on large companies, which can be cumbersome for smaller practices in terms of setup and integration.
- Enterprise-style (not published per-seat or flat-fee) pricing and contracts are the norm and might need to be negotiated on a custom basis.
Price:
quoted on request
Website:https://www.inovalon.com/insurance-discovery
8. Veritable
Veritable Insurance Verification Software is a specific healthcare technology that is customized to meet the needs of medical practices, billing companies, and hospitals to automate patient insurance eligibility checks and real-time claim status monitoring. It is seamless with electronic health record systems and practice management software, and it links to the majority of insurance payers, including all major commercial insurers, Medicare, and Medicaid plans in 50 states, to provide real-time coverage information, per-use co-payments, deductibles, and authorization requirements. It can minimize claim denials, quicken reimbursements, and improve the management of the revenue cycle.
Key Features:
- Check patient benefits, coverage status, and out-of-pocket costs on 1,000+ payers and 99% of the time.
- Prepare up to 5,000 patient records, batch verify them, and end up saving hours per day by eliminating manual data entry.
- Monitors a claim between submission and adjustment time, and sends notifications when it has been postponed or rejected.
- It can support X12 EDI, FHIR, JSON, or CSV exports; a personalized report of audits and billing.
- Establishes safe payment connections in co-pay and balances with the help of eligibility data.
- Web dashboard is operational in 15 minutes; it does not require IT implementation and is designed in a mobile-friendly format.
- EHR/PM integration (e.g., Epic, Cerner), AI-based detection of suspicious claims.
Pros:
- Rapid configuration and user-friendly interface.
- Completes major reductions in denials and AR days.
- Pay-per-use; Flexible; small to large practices.
- Good payer coverage and HIPAA.
Cons
- Less user reviews compared to the competitors, such as Availity.
- Ultra-high-volume users may be limited by the batch limits.
- With no volume offerings, pricing can easily add up for heavy usage.
Pricing
Plans begin at $50/month.
website: https://www.veritable.app
9. InstantVOB
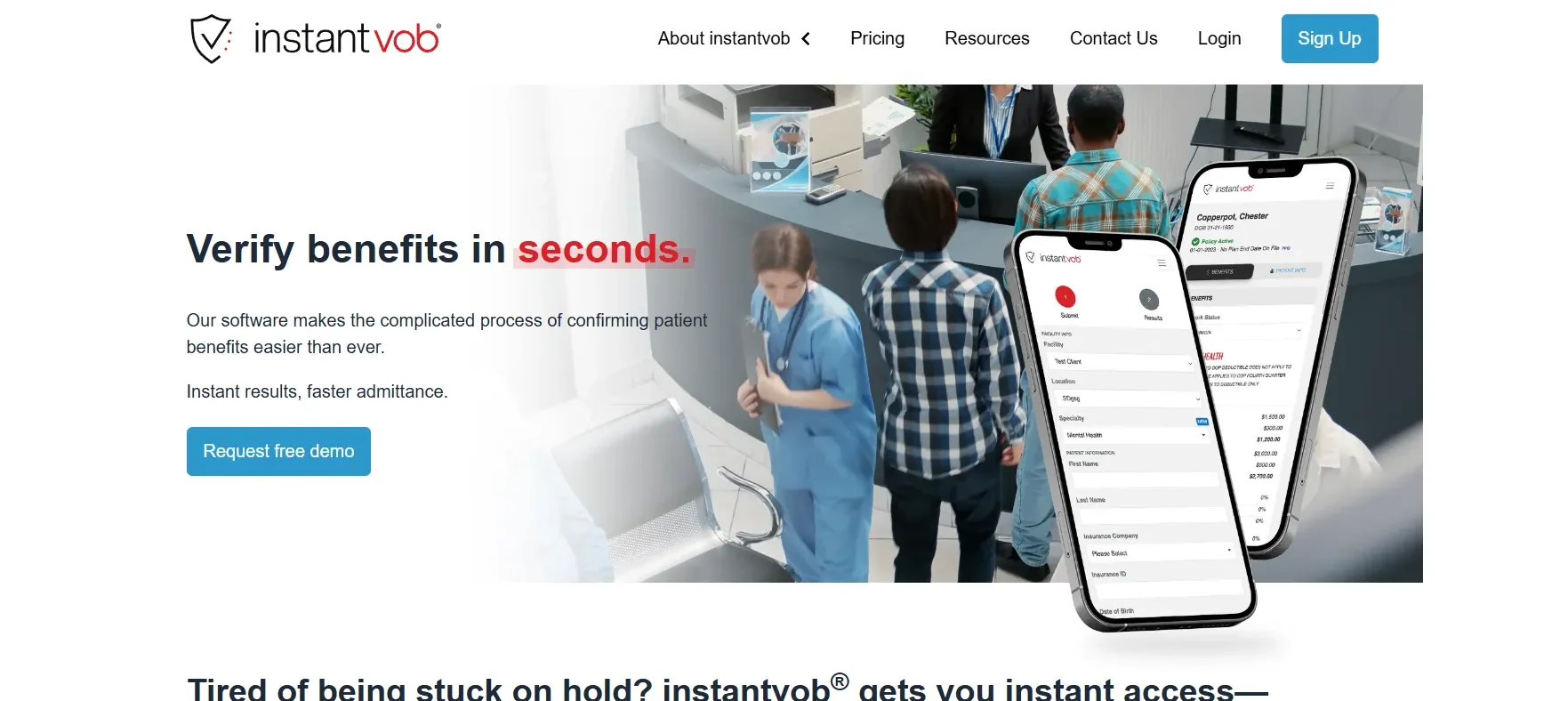
InstantVOB Insurance Verification tool is an automated, cloud-based software that assists healthcare professionals in real time, automatically, and quickly in nearly real time, checking the insurance status and benefits of a patient based on payer connections and extensive insurance databases. It can be combined with the current workflows like EHRs and billing systems, minimize manual phone calls and paperwork, and identify the coverage issues at an early stage to reduce claim denials and increase cash flow.
Key features:
- On-the-fly insurance eligibility and cover checks on the patients.
- Data entry and validation can be done automatically only with a few identifiers of the patient.
- Connectivity with various payer insurance databases.
- Expansion discovery to find coverage that can have been overlooked.
- Combination with EHRs, medical billing software, and other healthcare systems.
- Reporting and formats that are customizable for the eligibility and billing data.
- 24/7 access, data encryption, and access-control security are cloud-based.
Pros:
- Quickens eligibility checks and lessens front-desk workload.
- Enhances precision and assists in reducing the denials of claims and delays in payment.
- The pay-as-you-go pricing model has the ability to cut initial expenses.
- Operations in various locations and distant employee arrangements.
Cons:
- Depends on the availability of payers; it is not verified in case the payer system is offline or unavailable.
- Instant verification does not imply payment, and therefore, there is a certain amount of billing risk.
- May needs preliminary integration with the existing EHRs and workflows, and staff training.
Price:
- Monthly Subscription:$179.99/month
- Enterprise: Custom Pricing
Website:https://instantvob.com/
10 Clearwave
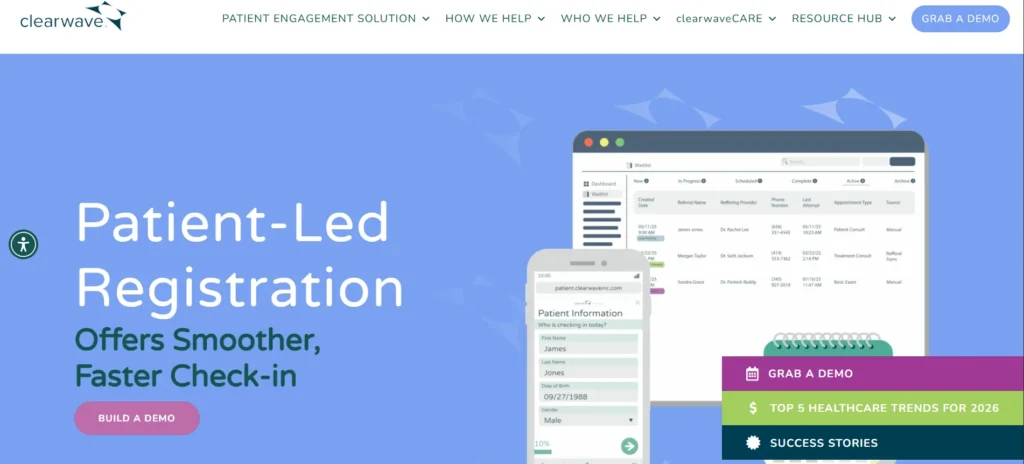
Clearwave Insurance Verification Software is a medical practice insurance verification and patient-revenue system available as a cloud-based application that is intended to automate insurance verifications, enhance point-of-service collections, and streamline check-in. It integrates with large clearinghouses and hundreds of payers, retrieving live eligibility information at various touchpoints of the patient, and front-office employees can show the correct financial responsibility, in advance or at check-in. Clearwave assists in minimizing claim denials, expediting payments, and improving patient experience through branded self-check-in, automatic reminders, and financial transparency by minimizing the use of manual verification and guessing eligibility.
Key features:
- Multi-factor insurance eligibility checks in real time with 900-plus payers.
- Automated eligibility at various points of contact (pre-visit, check-in, kiosk).
- Calculation of point-of-service co-pay and past-due balance, and collection.
- Patient self-check-in and kiosk checking in with built-in eligibility reminders.
- Eligibility discrepancy flagging and error resolving software to minimise claim rejections.
- Individualized branding and patient engagement services.
- Dashboard indicating real-time eligibility, deductibles, co-pays, and payer status.
Pros:
- Rapid insurance inspections and check-in which lessen the workload of the front desk.
- Enhances the quality of insurance data and reduces claims rejection.
- Develops point-of-service collections and capture of revenue.
- Improves the patient experience through self-check-in and open cost estimates.
- Interoperability with EMR/EHR and practice-management systems.
Cons:
- Pricing is not entirely transparent; it depends on the size of the practice and module.
- Other users report a learning curve to use all the features.
- Mainly serves physician practices but can also offer additional than minimum eligibility instruments.
Price:
quoted based
Website:https://www.clearwaveinc.com
11. QuickAdmit
QuickAdmit is an insurance-checking and eligibility-checking program primarily targeted towards behavioral-health and treatment-center admissions departments, and allows staff to check the insurance coverage of patients fast and dependably before or during intake. It provides real-time benefit checks on most commercial payers with a single sign-on interface, allowing team members to access coverage information and determine eligibility without having to manage multiple payer portals, and it allows 24/7 access to support the team in effectively managing after-hours admissions.
Key features:
- Real-time eligibility / VOB searches on any device, usually in a few seconds.
- 24/7 admission coverage of round-the-clock teams.
- Linkages to hundreds of business insurance payers via a single platform.
- Single blanket benefit payments on numerous payer databases simultaneously.
- Ready-made treatment and behavioral-health workflows.
- Auto-correction of patient-demographics to decrease data-entry mistakes.
Pros:
- Developed to focus on behavioral-health and treatment centers’ admissions processes.
- Eliminates the second call to provide first call instant eligibility responses.
- Decreases time in manual hold times and payer phone tree.
- Widespread coverage of payers is used to verify gains despite smaller patient records.
Cons:
- The smaller vendor, has a relatively small overall feature range in comparison with full-suite RCM sites.
- Not available with ERA posting or claim status tracking.
- Lacks proprietary financial-, or denial-, analytics tools, thus practice might require additional software.
Price:
The precise prices may be different depending on the size of the facility and the plan.;
website: https://www.quickadmit.com
12. AdvancedMD Eligibility Verification
The Eligibility Verification of AdvancedMD is a cloud-based insurance verification application part of its practice management and billing offering, which aims to simplify the process of checking the insurer of patients by automating the process of eligibility inquiries with medical, dental, and vision insurers with more than 1,500 carriers. It draws real-time coverage information such as copays, deductibles, and authorization, right into patient records, schedules, and dashboards, minimizing claim denials due to eligibility mistakes – problems that industry reports show are the case in 50% of medical claims. This tool is used to facilitate batch processing of scheduled appointments, modifiable rules, and a smooth write-back to the EHR of AdvancedMD, making it easy to improve front-office performance and revenue cycle management.
Key Features
- The patient schedules and next-day appointments are subject to batch eligibility checks.
- Live validation of coverages (copays, deductibles, coinsurance) automatically fills out patient charts.
- A business rules engine that allows customization of results, such as filterable Excel reports and issues alerts.
- Single-login access to billing, claims scrubbing, and denial management through integration with AdvancedMD.
- Price transparency through the use of all the information available on the fees and eligibility of patients.
Pros:
- Minimizes rejections and telephone calls.
- Simple installation and automatic notifications.
- Multi-payer support.
Cons:
- Pricing varies and can be high.
- Modular add-ons needed.
Pricing:
quoted based on
Website: www.advancedmd.com
Comparison Table: Insurance Verification Software
Conclusion
Insurance verification software is no longer optional—it is essential for healthcare organizations aiming to reduce claim denials, streamline operations, and improve financial outcomes. Manual verification processes often lead to delays, inaccuracies, and increased administrative burden, directly impacting both revenue and patient satisfaction.
By adopting automated solutions, healthcare providers can access real-time eligibility data, verify coverage with greater accuracy, and integrate seamlessly with EHR and practice management systems. This not only minimizes errors but also ensures faster claim approvals and smoother revenue cycle management.
With the wide range of tools available today, choosing the right platform depends on your practice size, specialty, and workflow needs. Investing in the right solution can significantly enhance efficiency, reduce operational costs, and allow your team to focus more on delivering quality patient care.
FAQs
Q1. Why Is This Software Relevant To Healthcare Practices?
These tools decrease the number of claims denied, decrease the time of registration, enhance the accuracy of billing, and decrease the number of manual follow-ups by providing the front-desk and billing staff with current insurance information before care is provided.
Q2. What Are The Main Characteristics Of The Most Suitable Insurance Verification Software?
Find real-time eligibility, EHR/EMR integration, multiple payer support, batch query, benefit information (copays, deductibles, maximums), and a convenient dashboard with coverage warning messages.
Q3. What Is The Role Of Insurance Verification Tools In Eliminating Claim Denials?
The software can save time by validating active coverage and proper plan details at the point of confirmation, notifying of missing prior authorizations, and exposing coverage limits or restrictions before the billing of services.
Q4. Does This Software Work With My Current EHR Or Practice Management System?
Yes, the majority of up-to-date insurance verification solutions include direct connectivity with major EHRs and RCM through APIs or built-in modules, allowing for the conduct of eligibility checks during the process of patient chart or registration.
Q5. Does The Software Work With Small Clinics And Also With Large Hospitals?
Yes, most of the solutions are scalable, providing straightforward web portals to small practices and advanced API based workflows to big health systems, with pricing and functionality based on the size and volume of practices.




